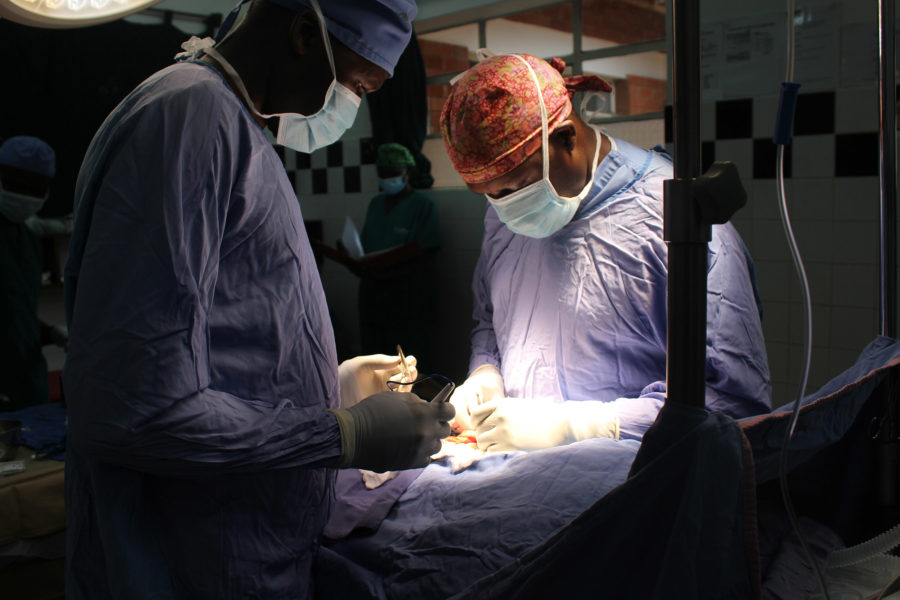
CURE International supports global surgery initiatives
In June 2019, the World Health Organization (WHO) wrapped up their 72rd World Health Assembly (WHA), which was held May 20-28, 2019, in Geneva, Switzerland. During the opening ceremony, Richard Horton, the editor-in-chief of The Lancet, gave an address, and in it he did something interesting. In the lead-up to the WHA, Horton asked this question on his Twitter account:
If you had 10 minutes to speak to 194 member states at the World Health Assembly, what would you say?
— richard horton (@richardhorton1) May 18, 2019
He received a lot of replies to his question (you can read the full thread here), which is to be expected. After all, there are often as many opinions as there are people, especially when topics as broad and multifaceted as global health are broached.
In his address to at the WHA, Horton read off the top five replies to his question on Twitter, and among these was to “invest in safe surgery and anaesthesia.”
The fact that this point about surgery was among the top five responses is telling – the access to surgical treatment and the importance of safe surgery and anaesthesia has become one of the more pressing issues in the debate around global health and universal health coverage (UHC). Although most of the focus (and funding) in global health has centred around the struggle against diseases such as malaria, tuberculosis and HIV/AIDS, in recent years this has begun to change. Surgery as an essential component of global health has started to gain traction in the public discourse, and has been supported by research. Through important publications such as The Lancet Commission on Global Surgery, and the World Bank’s Disease Priority Control 3, Vol. 1, there is a growing recognition of the fact that surgery is not only a cost-effective way of contributing to the overall health and development of a country – it is also an essential element of basic healthcare.
This last point is important. The WHO has made advocating for UHC one of their top priorities, especially as it relates to the UN’s Sustainable Development Goals (SDGs). Goal #3 aims to “Ensure healthy lives and promote wellbeing for all at all ages,” and this cannot be done without basic health coverage provided to all.
In an address to the global surgery community earlier this year, the Director General of the WHO, Dr. Tedros Adhanom Ghebreyesus, had this to say on the link between surgery and UHC,
“No country can achieve Universal Health Coverage unless its people have access to safe, timely, and affordable surgical services. Nine of the 13 targets in SDG3 will never be achieved without improved surgical care. And yet, globally, 5 billion people and 90% of the world’s poor lack that access. It’s therefore vital that countries invest in surgery.”
This topic will also be addressed at the upcoming High Level Meeting on UHC, which will take place on September 23, 2019, during the 74th session of the United Nations General Assembly in New York. The G4 Alliance and others are advocating for global surgery to be included in the discussion, and CURE International supports this effort.
This is directly linked to the work of CURE International—we understand the impact of providing surgical services to communities who usually do not have access to them, and we know how life-changing and transformative it is. We provide safe surgery and anaesthesia to patients in low- and middle-income countries, significantly reducing the global burden of disease imposed by conditions such as cleft lip/palate and burns, along with orthopaedic and congenital conditions. We also provide training to local surgeons and anaesthesiologist (as well as nurses, physical therapists, and other healthcare workers), and help to build the capacity of the healthcare systems of the countries we serve. Finally, we provide spiritual ministry which seeks to share the message of God’s love and to heal the emotional wounds that result from the trauma of living with a disability in a world where disability is misunderstood and often associated with inaccurate and harmful traditional beliefs. These wounds can persist long after the physical condition has been treated, and only by addressing them are we able to offer holistic healthcare, which sees the person as a whole and helps restore human dignity as well as functionality and mobility.
Footnote: Article written by Josh Korn on Saturday, June 1, 2019