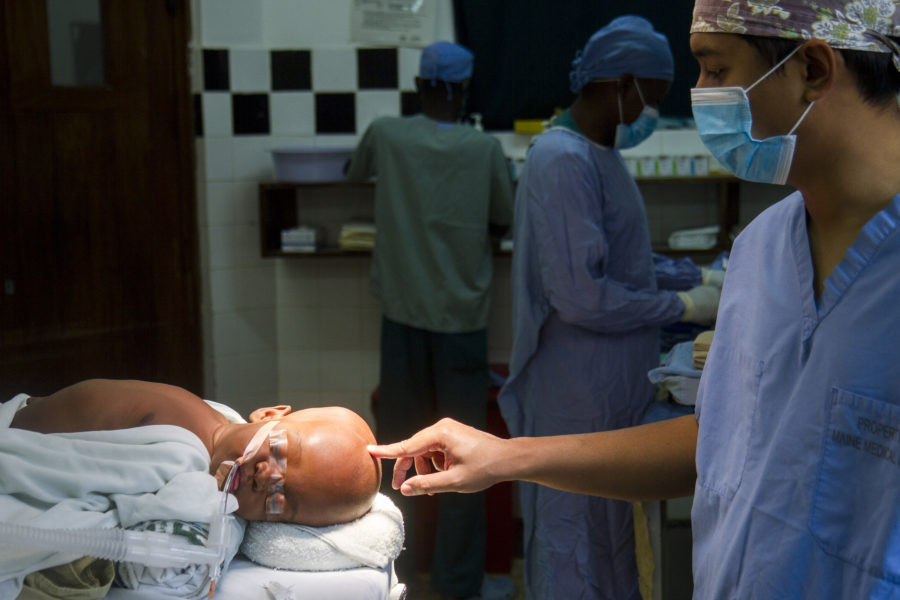
Dr. Mousa brings innovative ETV/CPC procedure to Indonesia
“In my hometown, neurosurgery doesn’t happen often,” says Dr. Mousa, a fellow in the CURE Hydrocephalus & Spina Bifida (CHSB) programme.
Dr. Mousa’s use of the word “hometown” may make you think of someplace small, but his Indonesian city contains a population of 7 million.
“There are many motorcycle accidents and also many paediatric needs for children with hydrocephalus and spina bifida,” he explains. “We can only do shunts (an implanted device) to treat hydrocephalus. But when you read the new journals from America or Britain or elsewhere in Europe, they say ‘the best shunt is no shunt.’ They mean no device! I wanted to try it. It is called ETV, but there is no equipment in my hometown.”
ETV/CPC is a fairly recent, innovative form of treatment for hydrocephalus. Developed by Dr. Benjamin Warf while treating patients at CURE Uganda, the procedure eliminates a lot of the long-term risk and expense associated with shunt-based treatment.
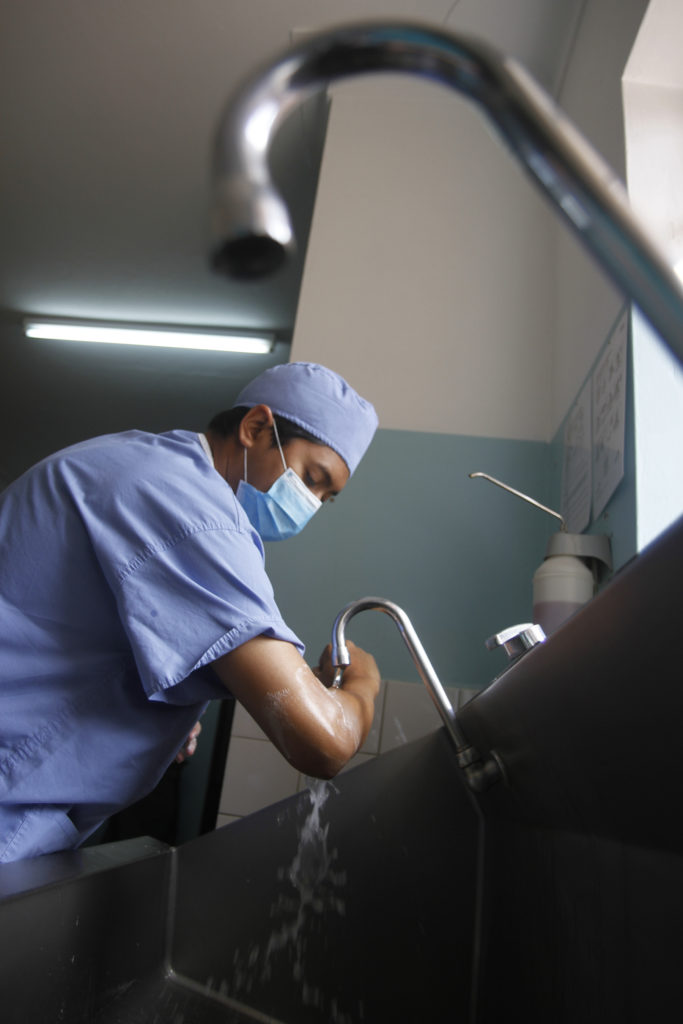
Dr. Mousa began researching the ETV/CPC procedure on the internet. At one point, he Googled “paediatric neurosurgery fellowship,” and the CURE website popped up. Intrigued by what he saw, Dr. Mousa reached out to Charles Howard (Operations Director for CURE Hydrocephalus and Spina Bifida) via email. After his graduation two years later, Charles offered him a fellowship at CURE Uganda.
Dr. Mousa was almost Businessman Mousa. He once had a scholarship to study business management in Malaysia. His parents had different a different hope for him; they wanted him to be a doctor, and they persuaded him to give it a try.
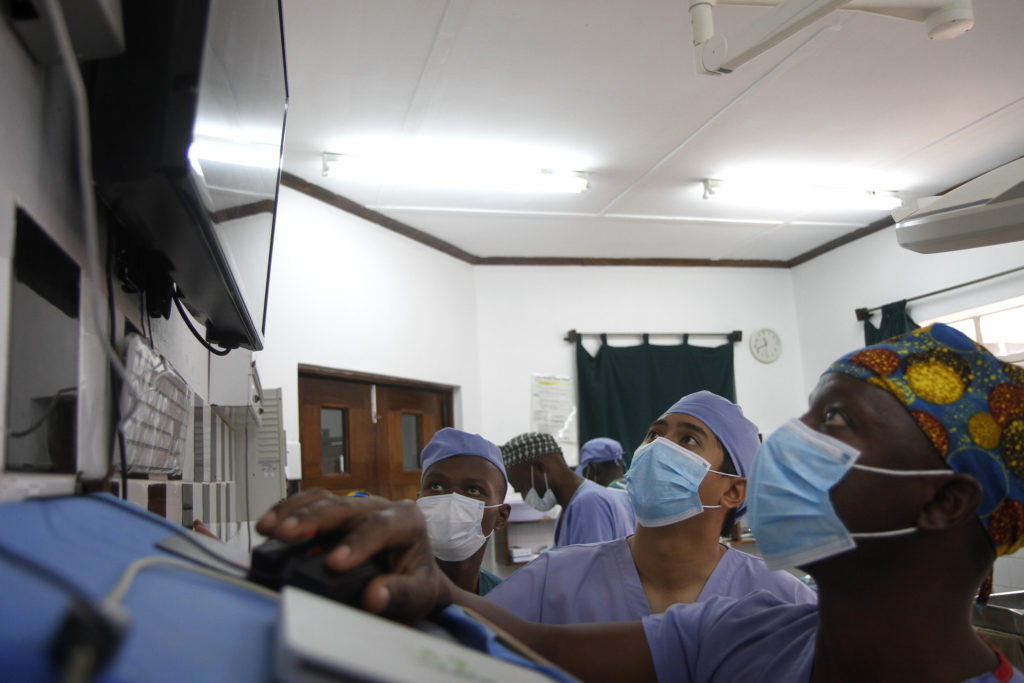
Nervous about the difficulty of pursuing a career in medicine, Dr. Mousa reluctantly took the entrance exam to get into medical school. He passed. He struggled through his first semester of medical school, even receiving a letter from the dean warning that if his grades didn’t improve, he would be asked to leave.
“Unfortunately, this letter is going to my mum, and my mum is crying. After that, I’m going to learn.”
His mother’s tears made all the difference. He studied hard and decided to specialise in neurosurgery.
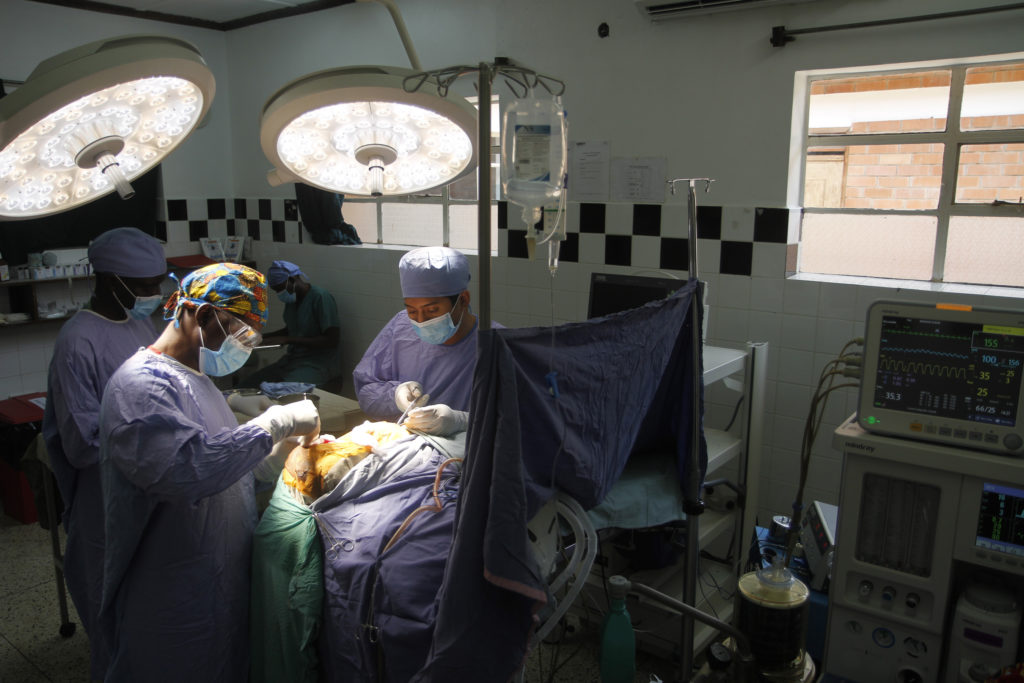
“I am always fascinated by how the brain works and how the brain anatomy looks.”
When he graduated from the neurosurgery program, his mother cried again. This time, she cried tears of happiness.
At the end of February 2018, Mousa travelled to Uganda to begin his six-week fellowship. Dr. Justin, Dr. Peter, and Dr. Mugamba taught him how to do the ETV/CPC procedure. The two-stage process first has the surgeon insert a flexible endoscope through a small incision on the patient’s scalp. A camera on the endoscope helps the surgeon to see inside the patient’s brain and locate the floor of the third ventricle, where he then makes an opening that allows the cerebrospinal fluid (CSF) to flow out of the brain, absorbed into the rest of the body.
The second procedure, the choroid plexus cauterization (CPC), has the surgeon cauterize the choroid plexus to reduce the amount of CSF that the brain produces. Together, the two procedures take the place of a shunt, a plastic tube that would be run from the brain to the abdomen to allow CSF to drain into the body.
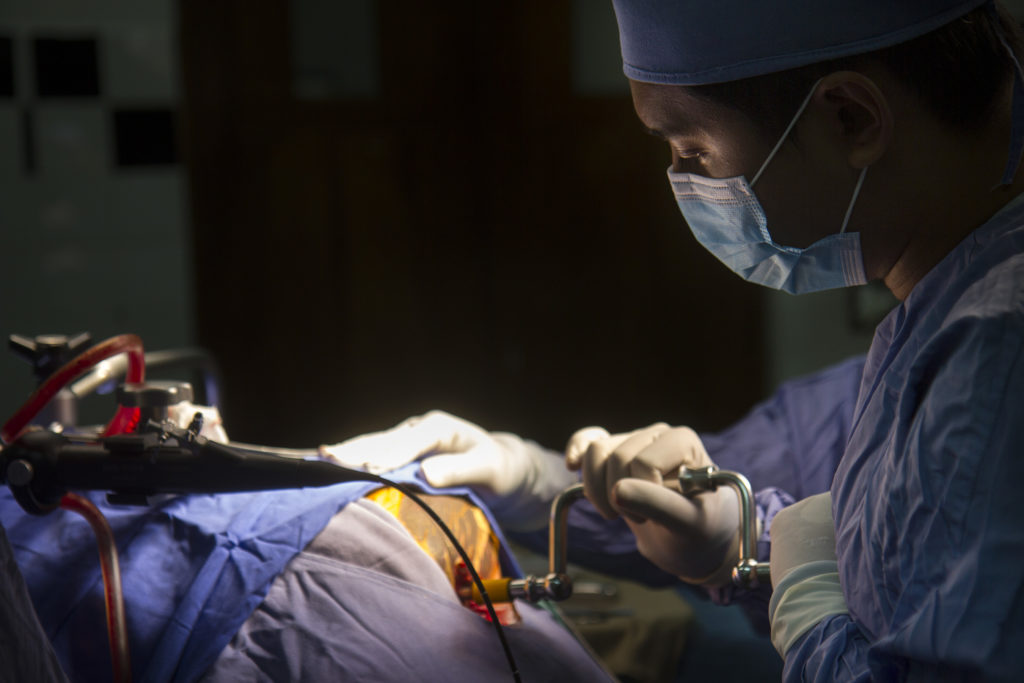
“My first cases, my hands were always shaking. I did not know the anatomy, still confused about the orientation, but now I can do the ETV without Dr. Justin beside me.” Dr. Justin observes Dr. Mousa from across the room.
“I want to be better,” Mousa insists. “I want to do better treatment for my community. Doing ETV (and not shunts) means a much better prognosis for the children in my country.”
Mousa praises the program, especially for how well they worked with him. He considers himself a slow learner.
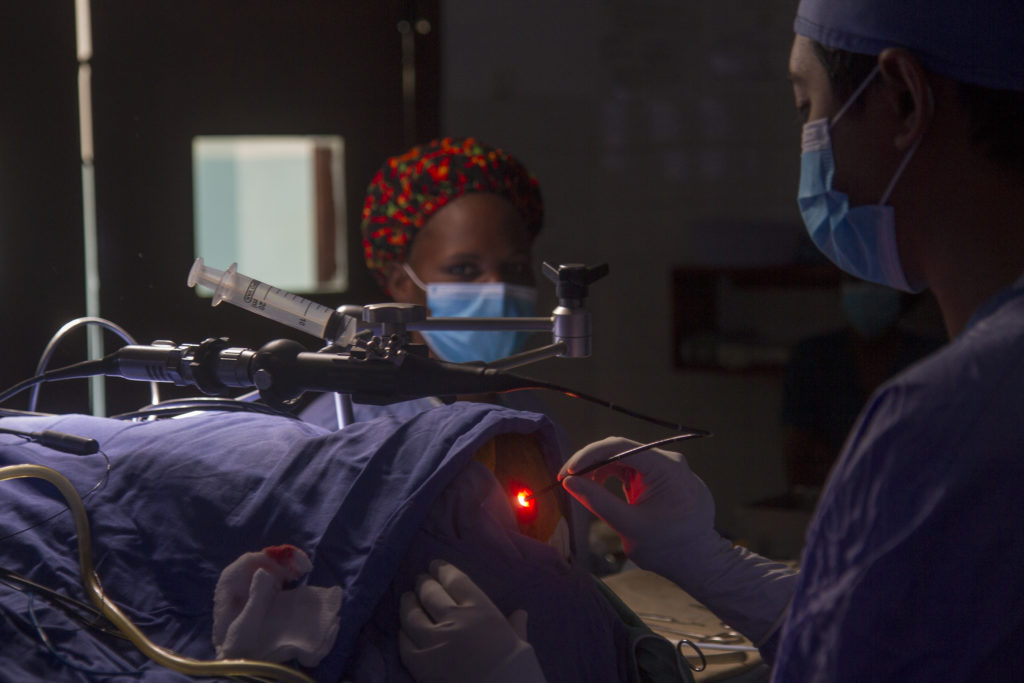
“They are always patient with me.” Dr. Mugamba and Dr. Justin encouraged him to take his time. Dr. Peter gently told him to “make your operation the best for the patient.” Mousa describes CURE Uganda as an environment conducive to learning, where the doctors calmly teach without judgment.
Dr. Mousa is excited about putting his training to use in Indonesia.
“I am hoping that with the knowledge from here, I can do much good in my hometown. I can do ETV,” he says, proudly.
For the children suffering from hydrocephalus within his hometown, that’s excellent news.
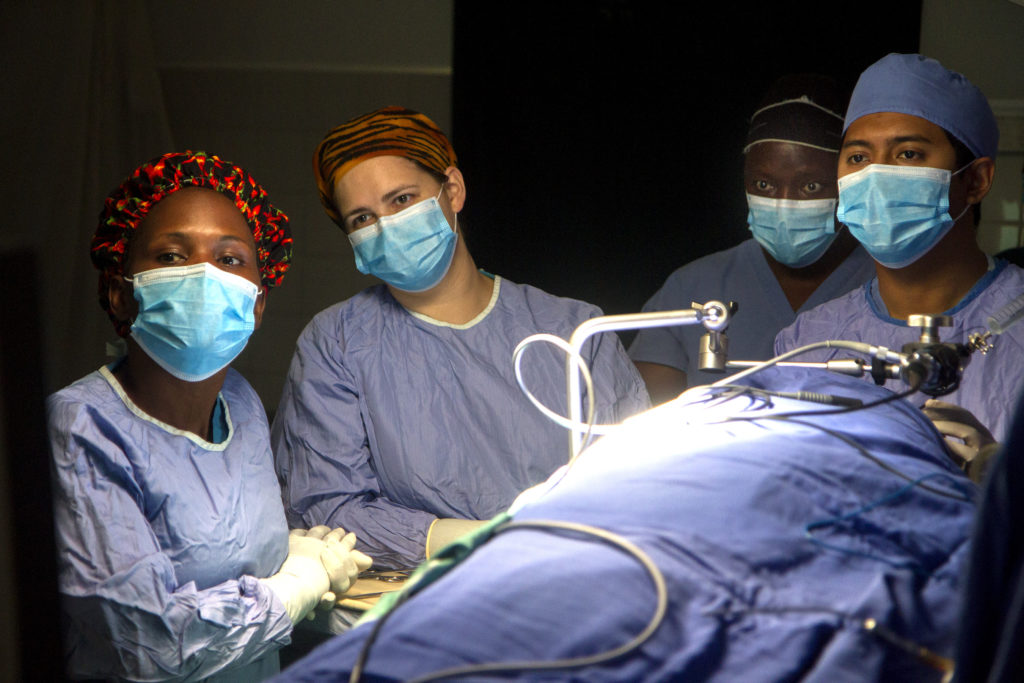
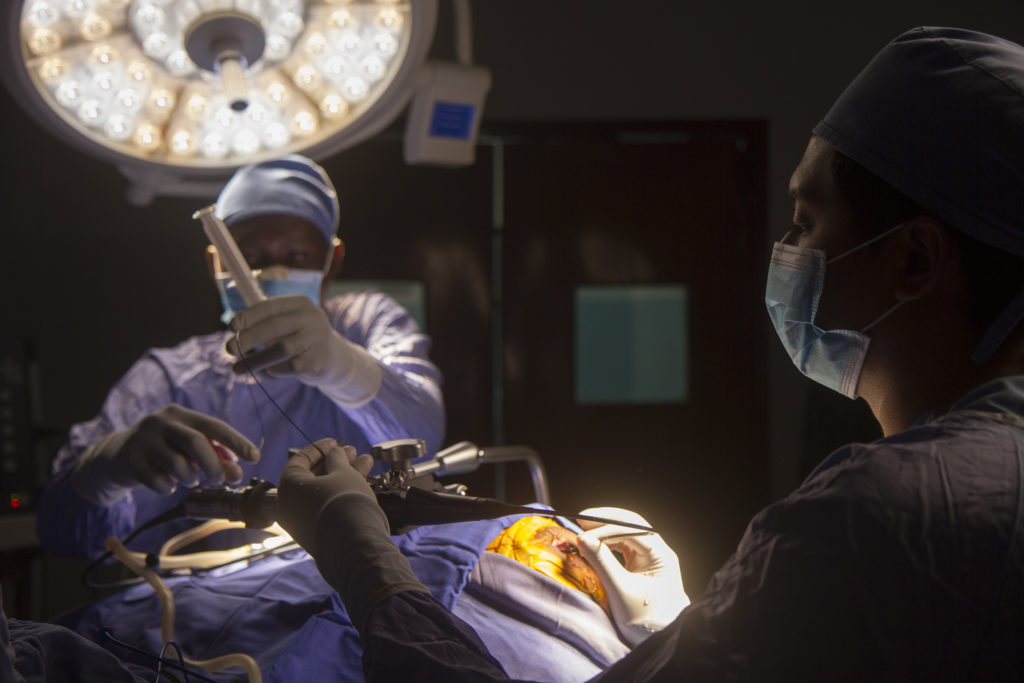
Footnote: Article written by Christopher Mullen