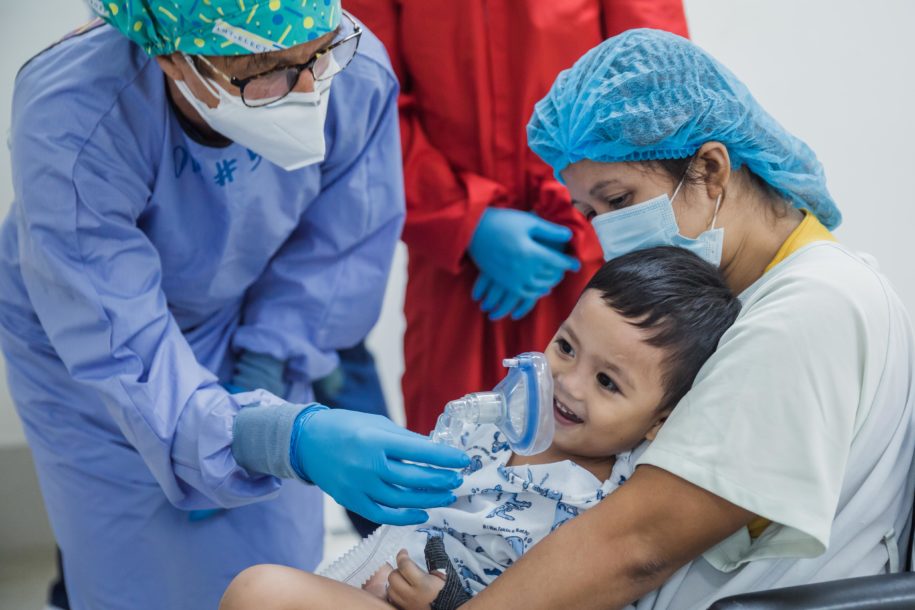
Safe Anaesthesia during COVID
On the 30th January, 2020, the World Health Organization (WHO) declared a public health emergency that was upgraded to a pandemic on the 11th March, and elective surgery such as cleft, ENT, and non-emergency orthopaedic surgery across the globe was put on hold, as hospitals had to battle with the influx of patients infected with the SARS-CoV-2 virus. In some places, operating rooms had to be reassigned as Intensive Care Units to accommodate patients with severe respiratory symptoms.
CURE has a network of seven paediatric hospitals across Africa and Asia that offer elective surgical care to some of the most vulnerable children and young adults in society. These hospitals form an integral part of each country’s healthcare services and provide valuable training for local surgeons and anaesthesia providers. As the virus spread across the world, leaders from all seven CURE hospitals met regularly to decide the best way forward. The decision was made to continue serving patients with increased safety protocols with contingency plans in place in case the local government hospitals were overrun and needed to use CURE hospital facilities.
During the first wave, the virus seemed to be moving rapidly across the globe, generating enormous fear with minimal understanding. The media amplified this fear with a huge emphasis on case fatality rates, and across the world, countries responded differently, and guidelines seemed to change daily: mask/no mask, aerosol vs. droplet spread, infectious for 2, 5, 7, or 14 days, and so it went on.
The positive side to the pandemic has been the readiness to share information across all countries, and numerous papers on the subject have been published, even though experts hold widely differing views. CURE realized that as an organisation it had to be well informed but also remain agile and flexible so that it could adjust its guidelines as new information became available and as the situation fluctuated across the different countries where CURE hospitals are located.
CURE hospitals are paediatric, surgical hospitals offering high-quality often complex surgery to children with disabilities and adults who would otherwise have no access to this care. This type of medical care, which may involve multiple surgeries and prolonged rehabilitation, allows these children to be reintegrated into society and lose the stigma of their disability. But successful high-quality surgery requires safe, high-quality anaesthesia. CURE has made every effort to create a network of hospitals that operate to a very high standard, despite the limited resources in the countries where they are located, and this is especially important for anaesthesia, which is a forgotten specialty in most low middle-income countries. Unstable electricity, intermittent water supply, unreliable delivery of oxygen, poorly maintained equipment, a shortage of drugs, and above all, a scarcity of qualified personnel hampers the delivery of safe and reliable anaesthesia. In Northern Uganda, there is an area where anaesthesia providers are called “the people who make you die a little,” as everyone is acutely aware of the potential dangers of anaesthesia in such a resource-constrained environment.
COVID-19 added another hazardous dimension to the provision of safe anaesthesia. The role of the anaesthesia provider is to ensure a pain-free surgery, often accompanied by a loss of consciousness, which means managing the airway and breathing of the patient. From the experiences of our Italian colleagues, it was evident that adaptations to the provision of anaesthesia and airway management would be necessary for staff and patient safety during the COVID pandemic. The willingness to learn and adjust was ever-present, but there was a palpable nervousness as many of us were scared, like watching a tsunami from the shore and waiting for it to hit. The anxiety stemmed largely from the risk of intubating patients. There was unease as none of us knew the actual personal risk, as frontline healthcare workers and airway managers. Tracheal intubation and facemask ventilation rank highly on the WHO list of aerosol‐generating procedures. How do hospitals proceed safely?
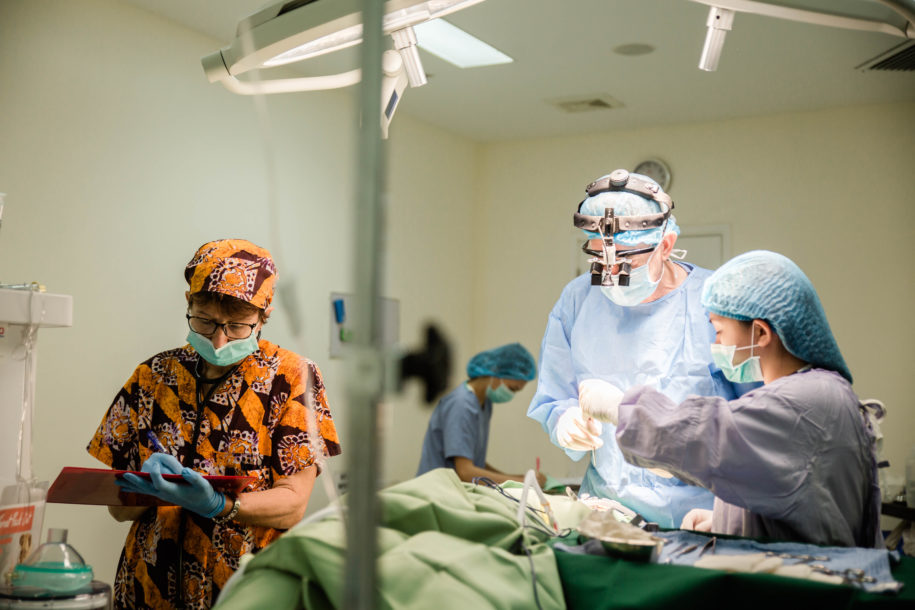
Senior management of all CURE hospitals met regularly to keep abreast of any new information, support each other, and provide clarity to hospital procedures and policies, which needed constant updating. Thankfully, all seven hospitals managed to stay open, with only occasional closings due to staff infection or local regulations. CURE hospitals have taken precautions to ensure that their operating rooms, wards, and outpatient areas are protected from any potential COVID positive cases. Everyone (staff, patients, and visitors) have temperature screening before entering the hospital, hands are washed, and a health questionnaire is completed. All patients booked for surgery must undergo a PCR test before admission. Mask wearing is obligatory, and in some countries, staff and patients also wear face shields. PPE gear is particularly important for the anaesthesia team managing the airway. There has been an increased use of regional anaesthesia, especially for orthopaedic surgery – although many of the young children still may need concomitant general anaesthesia and some form of airway management. Simple routine tasks have become more complex and riskier. The cognitive overload makes a normal operating list more arduous. As a result, the hospitals have had to invest in extra PPE and special equipment to sustain and bolster the safe delivery of anaesthesia to the patients and protect the staff.
The core of the high standards at CURE hospitals is the staff. They are the hospitals’ biggest asset and are essential to keeping the hospital safe. Due to COVID, routine tasks take longer and are more exhausting. So, it is important to increase patient numbers slowly, taking time to practice with new equipment, ensuring there is sufficient PPE, and supporting one another. Recognizing that people have different levels of fear and may require extra encouragement is imperative to preventing staff stress. Some staff may have additional concerns at home. For example, they may live in a multi-generational household with elderly or frail relatives who are at increased risk if they develop COVID-19 infection. Loneliness and isolation are more common than is often realized, and the spiritual ministry team plays a vital role in supporting patients, carers, and staff.
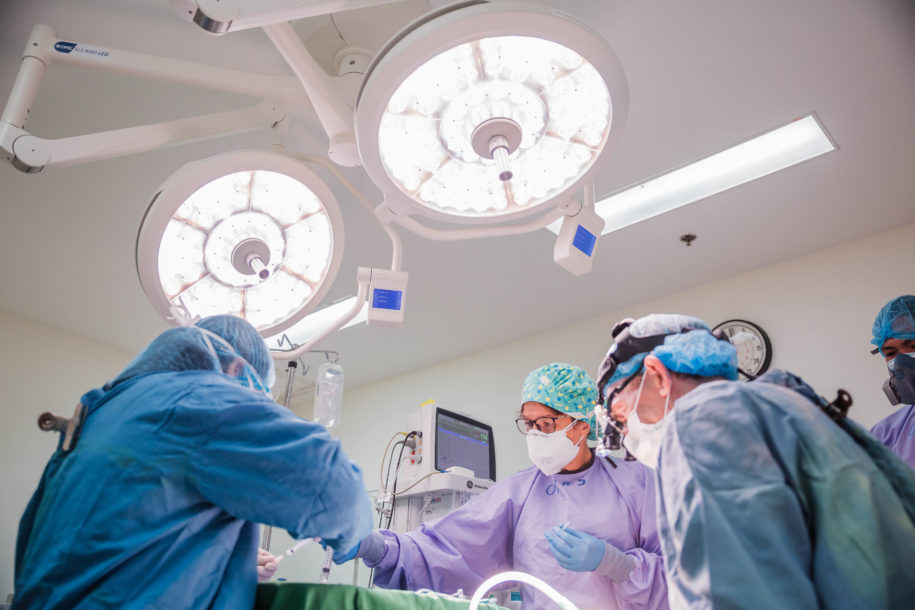
The entire CURE network is working tirelessly together to keep the hospitals open and functioning, delivering essential care to transform the lives of vulnerable children whose suffering would only be compounded by this pandemic. The measures that are put in place to protect our society and ourselves, especially health care workers, are very isolating. We must now wear masks – so you cannot see someone smile, stand 2m apart – so no chatting in the supermarket queue, and we are not able to shake hands in greeting. Even traveling for hospital treatment is restricted. All these important and necessary measures are distancing us from one another and preventing many from accessing essential care. We are social beings and do things together as groups, be it work, socializing, or leisure activities. Much of this is being prevented, and it is hitting the poor and defenceless the most. In this current time of “social distancing,” we need to be supporting one another – small acts of kindness and assistance can go a long way to help the staff continue working amidst the fear, risk, and restrictions.
CURE hospitals must stay open and functional to offer not only life-transforming surgeries but also to reflect the supernatural love of Jesus that transcends all boundaries and circumstances and is available to everyone.